 A couple questions that I received about C. difficile and hospital visitation dogs:
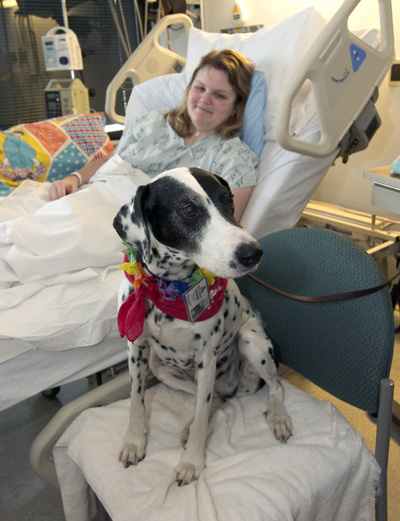
A couple questions that I received about C. difficile and hospital visitation dogs:
Is there any concern about cross contamination from dogs/handlers that visit health facilities and get contaminated by C. difficile? I see on this site a concern about dogs being contaminated by visitation and I wonder if the Delta Society has considered this to be an acceptable risk.
Dogs (and handlers) could be sources of C. difficile in hospitals. We have shown clearly that dogs that visit hospitals are at increased risk of shedding C. difficile in their feces, presumably because they ingest C. difficile spores from the hospital environment and/or patients’ hands. All dogs that go into hospitals are at risk, with dogs that lick patients and that are allowed up on beds at increased risk (Lefebvre et al 2009). We have also shown that the dog’s body can become contaminated with C. difficile after visiting a hospital.
Should there be a period of time mandated between visits to account for possible contamination?
That’s hard to say, but probably not. Contamination is a potential problem and certainly occurs, but we don’t know how long it lasts nor whether providing a "rest" period actually does anything. Clostridium difficile spores, the form of the bacterium that would be present on a dog’s coat, are very environmentally tolerant and can survive for years. Therefore, giving a few days break in between visitation would not result in the bacteria dying. However, some spores would presumably be physically removed over time, through shedding of hair, grooming and other activities. Based on that, it’s plausible that the longer the time between visits, the less likelihood of contamination still being present. Whether this actually helps, we don’t know.
What to do?
Among other things, we need to consider whether there is actually any evidence of risk. We don’t know whether dogs are able to transmit C. difficile in hospitals. My assumption is that there is some degree of risk, but it’s limited and can be controlled with good hygiene and the use of basic visitation practices, as highlighted in the "Guidelines for animal-assisted interventions in healthcare facilities" (American Journal of Infection Control, 2008).
Another thing to consider is whether there are any measures that can be taken to reduce potential risks, while maintaining a practical and effective visitation program. A key component of this is knowing that there are factors that make it more likely that a dog will be exposed to C. difficile during visitation. If a specific subset of dogs is at increased risk, then you have a clearer way to approach it. In this case, dogs that are allowed to lick patients and that are allowed on beds are at increased risk. These activities are modifiable – you can prohibit them without having a significant impact on the visits. Licking can be prohibited. Dogs can be kept off beds unless it is required, and when that’s the case, they can be placed on a towel or some other barrier to reduce their exposure to C. difficile from the bed. Additionally, we know that if a dog is being treated with antibiotics, it’s more likely to shed C. difficile, so dogs that are being (or have recently been) treated with antibiotics should be excluded from visitation.
For C. difficile to be a problem, it has to go from human or animal feces to a patient’s hands and then to a patient’s mouth. There are multiple potential interventions to interrupt this chain of transmission. At the end of the day, however, hand hygiene is the key. If people wash their hands before and after touching the dog, there should be much lower risk of disease transmission. A problem is that when I say "hand washing," I mean hand washing – not use of an alcohol-based hand sanitizer. Clostridium difficile spores are resistant to alcohol. That creates a conundrum because the use of alcohol hand sanitizers, a common and recommended hand hygiene method, doesn’t have the ability to kill C. difficile. Since not all visitation patients are able to get up and go to a sink, that complicates C. difficile control.