
“Doing nothing often leads to the very best of something.” ~Winne the Pooh
I don’t think the beloved wise sage of a bear was thinking about urine when he said that, but we can nonetheless heed the guidance of Winnie the Pooh when it comes to the management of subclinical bacteriuria. Here’s why:
Subclinical bacteriuria (also called asymptomatic bacteriuria in people) is a condition in which bacteria are present in the urine without causing any disease. In the past, this has often been considered something that needs to be treated, but we now know that the bladder isn’t always a sterile environment, and having some bacteria in it isn’t necessarily bad. Bacteria cycle in an out of the bladder, and subclinical bacteriuria is a common (normal) state for some animals (and people). We also now know that it rarely needs to be treated. In humans, the main indications for treatment are pregnancy and treatment prior to undergoing a urological surgical procedure. Unfortunately, it’s often treated unnecessarily (in both people and animals), which can lead to issues with adverse effects of antimicrobials, antimicrobial resistance, unnecessary costs and unnecessary hassles and stress.
When the first edition of the ISCAID antimicrobial use guidelines for urinary tract disease in dogs and cats (2011) was released, many people pushed back at the recommendation to not treat (or even test to look for) subclinical bacteriuria. By the time the second edition of the ISCAID guidelines for diagnosis and management of bacterial urinary tract infections in dogs and cats (2019) was published, there was a lot less resistance to this recommendation, but unnecessary treatment of this condition is still relatively common. As we continue work on the newest update to these guidelines, we hope for even better uptake, but realize that old habits die hard.
Subclinical bacteriuria is still often treated because of habit or fear. We need to focus on a few concepts to move past this out-of-date practice:
- We treat disease, not culture results.
- Not all bugs need to die.
- If a bacterium isn’t bothering my patient, it shouldn’t bother me (with rare exceptions).
- Doing something isn’t always better than doing nothing (even though we’re hard wired to think we need to do something). Listen to Winnie!
A new study in the Journal of Veterinary Internal Medicine (Le Corre et al, 2026) provides more support for Pooh’s clinical sense. It’s not earth shattering, and it’s not surprising, but it’s a really important part of providing more data help convince clinicians to leave it be.
The study is entitled Clinical outcomes and association with disease progression and survival of subclinical bacteriuria in cats with chronic kidney disease: a multicenter retrospective study. The researchers looked at 287 cats with chronic kidney disease, which is a population that’s at increased risk for subclinical bacteriuria. All the cats had urine cultures from samples collected by cystocentesis (i.e. using a needle and syringe to inserted directly into the bladder through the body wall to help reduce contamination of the sample), and none had any signs of lower urinary tract disease (e.g. straining to urinate).
- Bacteria were isolated from the urine of 38% of cats, which is pretty much in line with prior estimates of subclinical bacteriuria in this population. Unsurprisingly, female cats were 5.3 times as likely to have bacteriuria compared to males.
- Eschericia coli was the most common bacterial isolate, accounting for 68% of positive cultures, followed by Enterococcus (17%), Staphylococcus (5%) and Pseudomonas (5%). Twenty percent (20%) of bacteria were multi-drug resistant (ugh).
- Eighty-five (85) of the cats with subclinical bacteriuria were treated with antibiotics, of which 41% were treated before antimicrobial susceptibility data were available.
In cats treated with antibiotics, bacteriuria was identified again later on in 62% of them.
- That’s a key point. It demonstrates that treating the cats didn’t do anything to change their susceptibility to future episodes of bacteriuria, so it’s not surprising it happened again. This highlights the futility of treating this condition. If we eliminate the bacterium in the bladder today, odds are a new one will move in in the near future. The more we treat, the more likely we are to harm the cat (e.g. adverse events from the antimicrobial treatment), and the next time bacteriuria occurs, it may be resistant to our first line drug of choice. If the cat then develops an actual clinical infection that needs antimicrobials, we may have more limited treatment options.
When the researchers looked at 1500 day follow up in these cats, there was no association between subclinical bacteriuria and survival (see graph below). That fits with an earlier study of bacteriuria in senior cats, and with reams of data from human medicine.
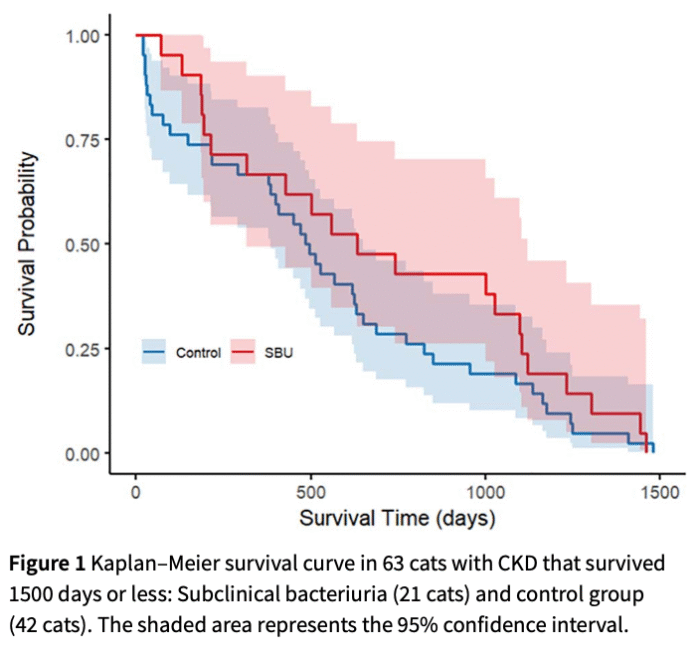
Progression of chronic kidney disease was also assessed in 134 cats. There was no difference in percentage of cats that showed progression of disease in the group with subclinical bacteriuria (42%) versus controls (40%). The detection of multiple episodes of subclinical bacteriuria was also not associated with progression of kidney disease.
There was no statistically significant difference between groups in the development of bacterial cystitis, though there was a numerical difference that’s worthy of further investigation That said, an additional question would be whether cats that were treated were more likely to have other complicating factors that were a driver for cystitis. There was also no significant increased risk of pyelonephritis in untreated cats.
All this supports the notion that subclinical bacteriuria is a common and typically benign state. Treatment can sometimes eliminate bacteria, but not always, and when it does, recurrence of bacteriuria is common. It’s possible that treatment would reduce the subsequent risk of bacterial cystitis, but even if there’s a small effect, we need to consider the potential adverse events associated with treatment, especially when treating lots of cats over and over again.
This was the researchers’ conclusion:
…we found no significant association of SBU with survival and disease progression in cats with CKD. Despite antimicrobial treatment of SBU in cats with CKD, urinary sterilization was not achieved in most cases, and progression to bacterial cystitis or pyelonephritis, although infrequent remained possible. Despite the fact that no clear guidelines for the management of SBU in cats with CKD currently exist, our results do not support routine antimicrobial treatment of this condition. Further evidence on the appropriateness of withholding treatment to manage SBU in cats with CKD remain however to be demonstrated before such recommendations can be made.
Image source: https://tommccallum.com/2021/05/21/doing-nothing-often-leads-to-the-very-best-of-something/