I’ve done countless presentations and interviews about COVID-19 and animals, and the question of whether pets can infect people always comes up.
My general line has been “We know that human-to-pet infection with SARS-CoV-2 is pretty common. My main concern is cats, since we know they can spread the virus cat-to-cat. If they can do that, it’s logical that they could spread it cat-to-person. However, it will be tough demonstrate. If a cat is infected, it almost invariably got exposed from someone in the household, and figuring out whether it was the cat or the infected person that infected someone else in the household (or a visitor) is almost impossible. The most likely way we’ll figure that out is if we see evidence of transmission in a veterinary clinic or shelter, where there’s no linked risk of human-to-human spread.”
A paper in the upcoming edition of Emerging Infectious Diseases (Sila et al. 2022) rounds out this discussion, providing strong evidence of cat-to-veterinarian transmission.
The story involves a 32-year-old veterinarian, two people with COVID-19, and their cat. Both owners had severe COVID-19 and were taken by ambulance on a 20-hour trip to the nearest available hospital bed. They had a cat and (I’d love to know how this came about) it rode along in the ambulance.
Upon arrival, the owners went to an isolation unit for treatment and the cat was sent to the university veterinary hospital, where it was examined by a veterinarian (and two colleagues).
The cat was healthy and the veterinarian collected nasal and rectal swabs for SARS-CoV-2 testing. In the process, the cat sneezed in her face. She was wearing an N95 mask but no eye protection. This is a common oversight – if there’s a high risk scenario where an N95 mask is needed, eye protection is almost always indicated. As a profession, we (veterinarians) do a pretty bad job of using eye protection.
I’m not sure how concerned they were at the time. The cat wasn’t known to be SARS-CoV-2-positive, and getting sneezed on by a cat isn’t exactly a rare event for a veterinarian (neither is getting drooled on, puked on, pooped on or close encounters with pretty much any bodily fluid… occupational hazard).
However, 3 days later, the veterinarian started to feel sick. She didn’t seek medical care until the results of the cat’s test came back 2 days after that – positive. She was tested and was also positive for SARS-CoV-2.
The timing is bang-on for cat-to-human infection, unknown exposure to another infected person had to be considered, so more investigation ensued. A veterinarian in the hospital’s large animal clinic also got COVID-19 around the same time, but there was no known contact between the two veterinarians, and the small animal veterinarian didn’t report any other known contact with an infected person.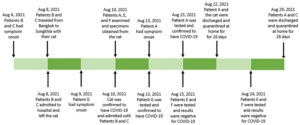
Here’s where genomics come into play. When they sequenced the virus from the two veterinarians, the two owners and the cat, they found that the large animal veterinarian had a different strain, so it was an unrelated infection. The strains from the cat’s veterinarian, the cat and the two owners were identical. Furthermore, that strain was different from strains circulating in people in that province (remember the owners came from 900 km away).
This was the perfect storm that allowed for identification of pet-to-human transmission or SARS-CoV-2: Exposure to an animal outside the household, where the virus strain involved wasn’t common (or even present) in the background transmission in the area, timely testing of people and the animal, and an ability to sequence all the samples.
The most surprising aspect of this report for me is that they had the right conditions to find zoonotic transmission, not that it actually occurred. I’ve been pretty confident it was possible, which is why we’ve done animal surveillance and spent a lot of time developing and communicating practical but proactive guidance to veterinarians to reduce the risk of just such an event.
Cat owners shouldn’t have much to worry about. The odds of a cat bringing SARS-CoV-2 into a household are really low. However, if it gets in via a person and the cat gets infected (which can occur ~50% of the time), we have to think about the implications for other people (and pets). If a household isn’t doing anything to separate infected and uninfected people, cats probably don’t matter much since human-to-human transmission is more likely. However, if households are separating those groups, include the cat. If I have COVID-19 and move to the basement to stay away from everyone, I should keep my cat away from me too (or keep it with me and away from everyone else). It’s also a reminder that we should continue to query COVID-19 exposure status of veterinary patients, and ideally postpone elective visits for cats from households with COVID-19. Emergencies are a different story, and we can take precautions to reduce the risk, but it’s preferable to bump an elective appointment.
All this relates to cats… what about dogs?
The risk from dogs remains unclear but is probably very low. We don’t have evidence of dog-to-dog transmission, and viral loads in infected dogs are typically low. I don’t think we can say there’s zero risk, but the risk is likely much lower compared to cats.