As someone who works a lot with infectious urinary tract disease in animals and has led urinary treatment guidelines, I guess it’s fitting that my dog got an infection.
To start, I’ll slap myself on the wrist for saying it was a urinary tract infection (UTI). We’ve been trying to improve the terminology in this field by using more precise terms. His specific issue was bacterial cystitis. I’ll use that for the rest of the post, but since UTI is commonly understood, I still use it for some audiences, for now at least.
Ozzie’s peeing predicament
Regular followers of the W&G blog have read about Ozzie more than once in the past. He’s a now almost-3-year-old (and definitely obnoxious) neutered male Labrador retriever.

The male part is relevant. As in people, bacterial cystitis in dogs is most common in females. However, that doesn’t mean that males can’t get bacterial cystitis, or that something particularly unusual is going on if they do. It’s just less common.
Oz also has a risk factor for infectious diseases: He has atopy (environmental allergies) and is therefore on oclacitinib (Apoquel), a drug that’s meant to modulate his immune system to reduce the allergic response, but also causes some degree of immunosuppression. Dogs on this drug aren’t severely immunosuppressed, but there is some increased risk of infection. It’s hard to say if that played a role here, but I suspect it did.
Back to Ozzie’s predicament
Oz went out in the morning and had a big pee. He then urinated small amounts a few more times. Then, throughout the morning, he kept going out to urinate small amounts. He’s a “grass is greener on the other side of the door” dog, who constantly wants in or out, but this was extreme, even for him, and the urination was abnormal. Since he was peeing a lot, it was easy to get a sample – it was turbid with a reddish tinge and some blood clots. That’s clearly not normal.
Stranguria (straining to urinate), pollakiuria (frequent urination) and abnormal-appearing urine scream “bacterial cystitis” but that’s not the only possible cause of these signs. We also always need to bear in mind that there can be other underlying issues (e.g. bladder stone, tumour) that may need to be addressed. That said, common things occur commonly. The fact that he’s male brings in some concern, but run-of-the-mill infections happen in males too, and his oclacitinib treatment provided a potentially straightforward explanation for an uncommon situation.
I looked at the urine under a microscope and there were lots of red blood cells, white blood cells and cocci bacteria within the white blood cells, all of which are supportive of bacterial cystitis involving a Staphylococcus sp.
Then the question becomes “to culture, or not to culture?” In a perfect world, we’d always do a culture. However, culture is expensive (very expensive in some places) and the value of the culture has to be considered. I want to do a culture when I’m not confident in what’s going on, when the odds of empirical treatment failure are high and/or when the implications of treatment failure are high. Let’s break those down.
What’s going on?
At that point, I was pretty confident Ozzie just had bacterial cystitis. While he could have something going on at the same time, odds are he didn’t, and culture wouldn’t really help me figure anything out at this stage.
Treatment failure potential
Since we have good guidelines for treatment of infectious urinary tract disease in pets from ISCAID (Weese et al. Vet J 2019) to help us pick approrpiate initial (empirical) antimicrobial therapy, the issue with treatment failure revolves around antimicrobial resistance. Resistance can occur in any infection, but in a young dog with no previous antimicrobial use history, no raw meat or raw treats in his diet, no hospitalization (apart from when he was neutered 2 years ago) and no contact with people that are likely to be shedding a antimicrobial resistant bugs, the odds of him having a resistant infection are really low. So once again, not much value in doing a culture for that reason.
Treatment failure implications
The question I ask regularly is “what will the status of this patient be over the next few days if I guess wrong with my antimcrobial?” If the answer is “likely dead,” I really want a culture and I really want to be confident in my initial drug selection. For Ozzie, the answer is simply “still uncomfortable and peeing a lot.” I’d rather not have that, but the in the grand scheme of things the implications of treatment failure are low. If the initial drug doesn’t work, we have lots of runway to figure out what will work before Ozzie’s in any serious trouble.
Generally I’d like to get a culture done routinely in cystitis cases, but for understandable infections that seem pretty run-of-the-mill in patients at low risk of a resistant infection, I’m fine with empirical treatment (as is common practice in people too).
That said, I did a culture anyway (more out of curiosity than anything else).
Next, I did exactly what we do NOT want people to do: I found some leftover antibiotics in the house and gave that to Ozzie. (Merlin, our previous Lab, had a root canal at one point and was sent home with 14 days (!!!) of antibiotics that we used for a total of 0 days… ignoring instructions from their veterinarian is another thing we do NOT want dog owners doing, but I’m pretty well versed in this area so I changed the treatment).
So Ozzie got amoxicillin-clavulanic acid for 5 days. If I’d had to get a new prescription for him I would have just used amoxicillin, but it was Sunday and I’m lazy, and amox/clav is also a recommended first line drug.
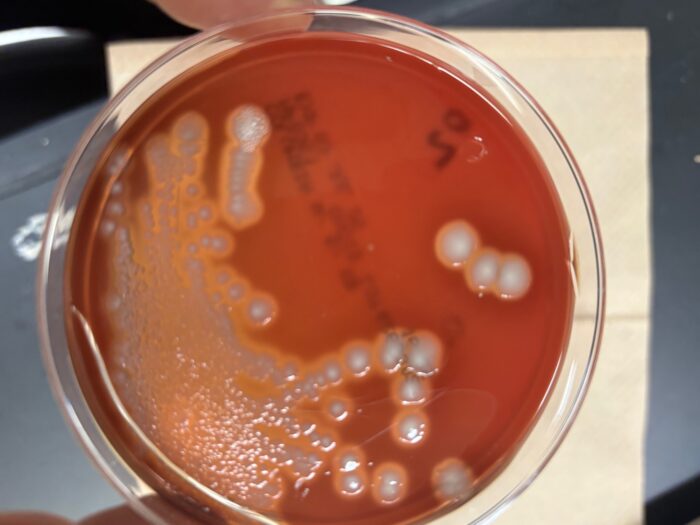
The next day, Ozzie was already looking better. He was peeing less frequently and his urine looked pretty good. There was still a bit of blood, as you can see by the little pellet of red at the bottom of the tube in the picture below. I checked the culture and could already see heavy growth of bacteria. The picture second picture below is the culture plate after 48 hours, which shows a nice, heavy, pure culture of Staphylococcus pseudintermedius.

Ozzie finished his antibiotics and… that was it. He responded well and there wasn’t a need to do anything more. If he relapses, then we need to do more investigation to see what else may be going on, especially since he had a staph infection, which can be associated with development of struvite bladder stones. But, our treatment goal was a healthy dog and since I got that, that was the end. So far, so good since then too. It’s been a couple weeks and he’s had no further issues. Hopefully it was a one-off infection, but we’ll see what happens.
The other thing we want to consider in any infection is whether there’s a risk factor we can mitigate to prevent it from happening again. Here, it’s tough. We could stop his Apoquel, but then he’ll be itchier (uncomfortable) and prone to secondary skin infections from scratching himself. His atopy is fairly seasonal though, so we can get him off treatment for a good part of the year, which helps.
Ozzie was a pretty straightforward case, which is actually a reason to talk about it. We tend to focus writing and and reporting and talking on the weird and wonderful, but routine disease causes most of the problems. Thinking about how we handle those cases is really important, but easy to overlook because they’re so routine.