For a parasite that rarely causes disease in people, the raccoon roundworm Baylisascaris procyonis gets excessive attention. I get an email every few days from people who are worried because:
- a raccoon pooped on their deck/garage/yard
- they found a raccoon latrine on their property
- they found unidentified feces floating in their pool
- they ran over a raccoon with their car
- just saw a raccoon walking across their yard
These scenarios all come with different degrees of risk, from zero to low. That said, the reason it gets so much attention is because in the rare instances it does cause infection, the disease can be severe and have long-lasting consequences. Like a lot of zoonotic infections, kids bear the greatest burden of disease; with B. procyonis, that’s because they are more likely to put things in their mouth that may be contaminated with parasite eggs from raccoon feces.
Here are a few quick facts about B. procyonis to keep in mind:
- It’s a roundworm that lives in the intestinal tract of raccoons.
- It’s very common in raccoons in North America and is expanding in Europe since the introduction of raccoons (along with the parasite). If you have raccoons in your area, you almost certainly have B. procyonis too.
- It’s generally harmless to adult raccoons. It probably mainly causes disease in young raccoons with large worm burdens.
- Raccoons poop out large numbers of B. procyonis eggs all the time. Once these eggs have matured in the environment for a few days, if a person ingests them, the eggs can hatch and the larvae then migrate through the body. Since we’re not raccoons, the larvae don’t know where they’re going, so they can migrate just about anywhere and can cause tissue damage in the process. The damage can be particularly devastating if the reach the eye (ocular larva migrans) or brain (neural larva migrans).
- Dogs can be infected with B. procyonis too. It’s rare, but sometimes they can develop the intestinal infection with mature roundworms after eating raccoon eggs. In that event, they pass eggs in their feces, just like raccoons do. Fortunately, routine dewormers easily eliminate these roundworms in dogs.
Now onto the real story (Moe will complain that I’m already writing too long of a post and I haven’t even gotten to the main event, but some background is good).
A couple of weeks ago (yes, I’m behind, it’s been a busy month), there was a report of B. procyonis infection in two (unrelated) children in Los Angeles County, California. The cases are pretty typical, but still worth highlighting.
Case 1 was an adolescent with autism spectrum disorder who had a history of pica (eating non-food items). He was hospitalized because of progressive behavioural changes, sleepiness, decreased activity, confusion and abnormal gait. As part of what I assume was a very extensive workup, eosinophilia (an increase in a certain type of white blood cell) was noted in a blood sample, which suggests some type of parasitic infection. Eosinophilia was also noted in a sample of spinal fluid, which essentially screams “neurological parasitic infection.” An ocular exam also identified a parasite larvae in the back of the eye. The image below (not from this patient) shows what this looks like.
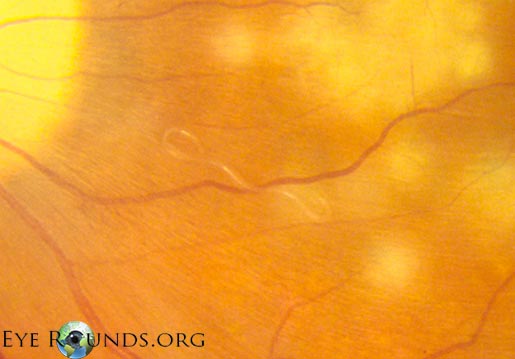
These findings, plus the changes noted on MRI, lead to a very solid presumptive diagnosis of B. procyonis infection. This was confirmed later through detection of antibodies against the parasite in the patient’s blood.
Laser treatment was used to kill the parasite in the eye, and a combination of albendazole (an antiparasitic) and a corticosteroid (to reduce inflammation) was used to treat the neurological component. Very fortunately (since this is often a devastating disease that causes irreversible damage), the child made a full recovery.
The family’s property was investigated to look for a source of infection, and a raccoon latrine was identified on a rooftop, which allowed feces to fall to the ground. Since the child had a history of pica, it’s assumed that he ingested feces or contaminated soil from that area.
Case 2 was an otherwise healthy 15-month-old child who was hospitalized because of acute onset of neurological disease, with weakness, altered gait and changes in muscle tome. Profound eosinophilia was noted in the blood and spinal fluid, but it doesn’t seem like parasitic disease was flagged at that time. A wide range of treatments for different possible causes was implemented initially, none of which included anti-parasitics.
Three months later, the child was taken to a follow-up appointment where he happened to be examined by the same doctor that treated Case 1. An ocular exam was performed and a parasite larva was seen. He was then finally treated with albendazole and corticosteroids. He also had antibodies against B. procyonis in his blood, rounding out the diagnosis. Unfortunately, this patient had serious neurological sequelae, possibly due to the delay in diagnosis and treatment. The eosinophilia should have been a trigger to think about parasitic disease, but it’s not clear why that wasn’t explored. Even with prompt treatment, the prognosis can be poor, but with late treatment, it’s worse.
No source of infection was found at the home of case 2, but raccoons were known to be present in the area. The child had been noted to put soil and bark mulch into his mouth, so presumably this is a really rare and really bad luck situation where a raccoon had defecated in the same area or where the mulch was obtained.
Take-home messages
- Raccoons should be discouraged from hanging around homes. Not feeding them and preventing them from accessing any food source are key steps (and also helps avoid other diseases raccoons may carry, like rabies!).
- People with a tendency to stick things in their mouths outside (including soil and feces) are at higher risk of infection. Proper supervision is important. If someone like that lives on or visits the property, there should be extra efforts to prevent raccoons from entering in the yard, and the yard should be inspected regularly for animal feces.
- Raccoon latrines should be properly cleaned up and efforts should be made to prevent raccoons from coming back to use them.
- Physicians need to have better awareness of zoonotic diseases in general. It’s hard to improve education about oddball diseases like this, but an obvious flag for potential parasitic disease seems to have been missed.
Jason Stull and I recently did a scoping review of human B. procyonis infections. It’s not open access until October, but I’ll write a follow-up post soon highlighting the main findings.
Image from eyerounds.org (University of Iowa)