Another emerging disease we’ve been paying attention to lately is canine lungworm. Lungworm is a generic name for infection caused by one of a few different parasites that live in the respiratory tract. A variety of different lungworms can cause disease in different species, and there tends to be a lot of regional variation.
Recently, lungworm cases have been identified in dogs in Ontario. For more details about the geographical distribution, go to WormsAndGermsMap.com (use the filter box on the left side to select lungworm). You’ll see cases distributed over a wide range of the southern and eastern parts of the province. Lungworms (Crenosoma vulpis, the fox lungworm, and Angiostrongylus vasorum, the“French heartworm”) are already well known in Atlantic Canada, but the movement into Ontario seems new.
So far, only Crenosoma vulpis has been found in Ontario. That’s good since it’s a less severe and more readily treatable parasite than A. vasorum, the other one we’re worried about entering the province.
As with many parasites, Crenosoma vulpis has a life cycle that involves multiple species (see the picture below from Bayer Animal Health). Foxes are the normal host. The adult parasite lives in the bronchi (large airways in the lungs). Their larvae move up the trachea (windpipe) to the mouth and are swallowed. These tough little larvae survive the entire intestinal tract and are passed in feces. When ingested by a snail, they continue to develop, and foxes are infected by eating snails. After ingestion, the larvae penetrate the wall of the stomach, get into the bloodstream and travel to the lungs, where the whole process starts again.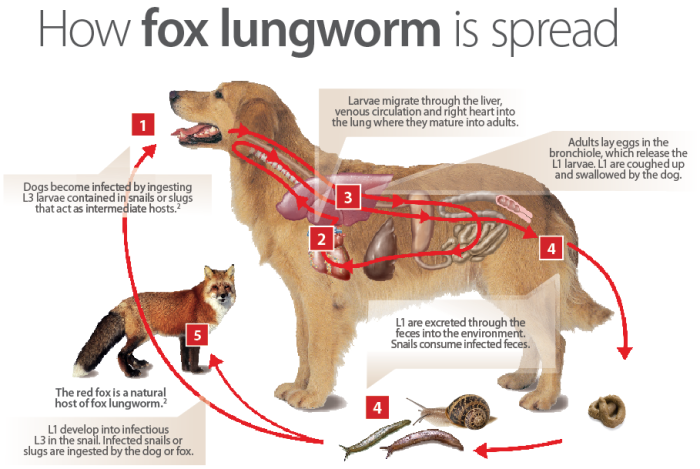
As close relatives of foxes, the same thing happens in dogs that eat infected snails (probably something that occurs more often than people like to think). Disease tends to be mild; most often a chronic cough caused by inflammation in the bronchi where the adult parasite hangs out.
Now that we know this parasite is present in Ontario, it’s something that should be considered in dogs with chronic cough. Diagnosis involves finding C. vulpis larvae in feces, usually through a “Baermann” test, which looks for parasite larvae (as opposed to a standard fecal flotation test that is used to look for parasite eggs from intestinal worms).
The good thing about lungworm, at least Crenosoma, is that it can be treated with antiparasitic medication and the prognosis is very good. The key is considering it as a possible cause so that a diagnosis can be made. That can be a challenge with emerging diseases when people don’t think about them.
Surveillance through veterinary clinics is ongoing to find out where lungworms are in Ontario and how often they cause disease.









