
That headline might get some people worked up, but hopefully they’ll read the whole post before firing off an angry email.
Antimicrobial resistance (AMR) is a huge problem in humans and animals, which means we need to improve or optimize how we use antimicrobials, but this is not synonymous with reducing use. Most of the time, improving and optimizing antimicrobial use (AMU) does focus on reduction, because we greatly overuse these drugs in general. Most of the national and international discussion around AMU also focuses on reduction, typically based on one quite crude measure: mass (kgs, tonnes) of drug used in animals over time (e.g. annually). Overall mass of drug used is usually one of the easier numbers to get (though even that can take considerable work depending on the system), and sometimes its useful, but it’s not always the best. Other times it’s simply not helpful, and other times it’s downright misleading.
I wrote a more detailed commentary on this same topic that was recently published in the Canadian Veterinary Journal, but here is a quick summary of some of the reasons why we need move beyond looking at simply reducing the mass of drugs used when it comes to improving antimicrobial stewardship.
All antimicrobials are not created alike
We have a lot more concerns about resistance to some drugs (higher tier) compared to others (lower tier). That’s why antimicrobials used in animals are categorized based on their potential impact on AMR in humans. Simply measuring the mass of all the drugs used together doesn’t consider which drugs are being used. It’s also important to account for differences in dosing. Newer, broader spectrum, higher tier drugs tend to be more potent, so they are used at lower doses (see table below), but the consequences of resistance to these drugs is much higher.
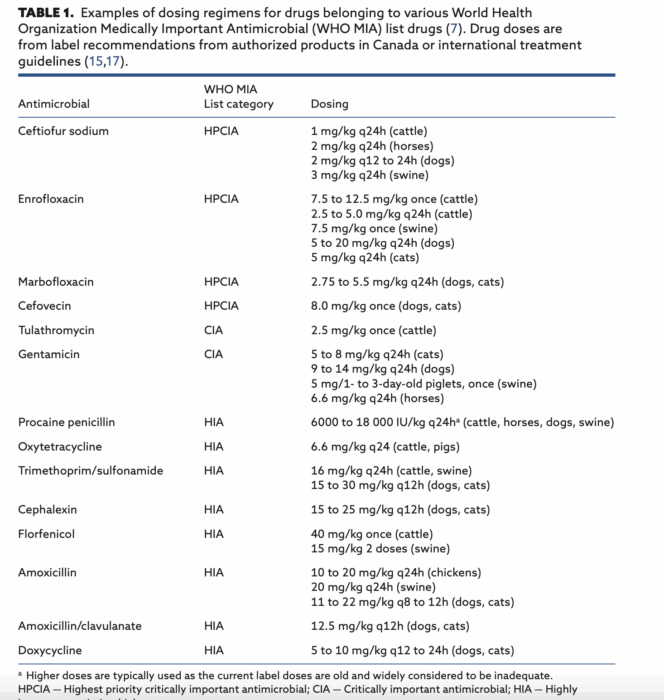
Based on this, we could significantly drop the mass of antimicrobials used in animals by using more higher tier drugs in place of lower tier drugs – but that is exactly what we don’t want to do! If a country is pressured to reduce AMU, the risk is they may simply substitute higher tier drugs for lower tier drugs, and then say “look how much we’ve reduced our antibiotic use, good for us!” while ignoring the disaster in the making.
Related to this, an increase in the mass of antimicrobial use might be good in some situations. Let’s use dogs with urinary tract infections as an example. In the table below, the “pre-intervention” column is based on 1000 dogs treated as per a study of AMU practices in dogs with urinary tract disease in the US and Canada. If we implement an intervention to move practices to 100% compliance with ISCAID guidelines for treating urinary tract disease in dogs, it would increase the use of three lower tier drugs, which is good. But, it would also increase the overall mass of drugs used by quite a bit, based on how they are dosed. Looking at the effect on mass of drugs used alone makes this look like a harmful intervention, when in fact the change would be good from a stewardship standpoint, since it would mean using the lower tier, recommended drugs.
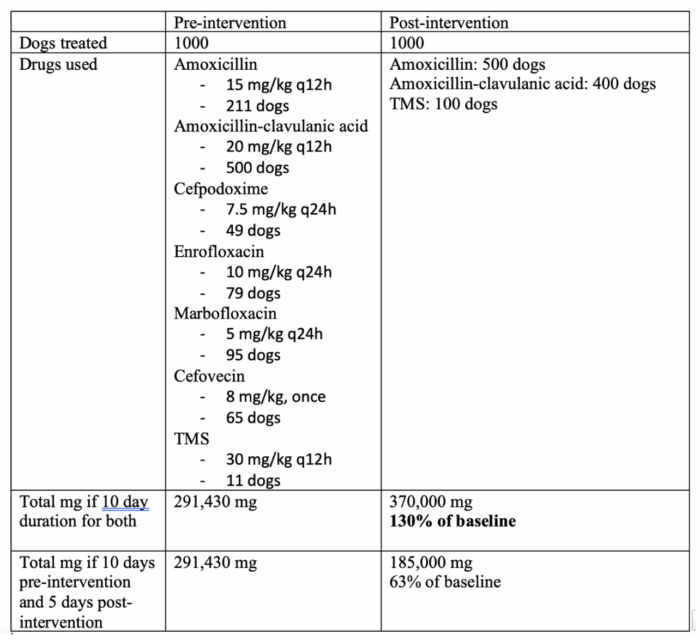
Increased animal production
The world is growing. Populations in some countries are expanding greatly, and overall wealth is increasing, leading to more need for food, and more demand for meat. We can debate the ecological aspects of meat production, but ultimately we can’t expect countries to stop increasing their own food production to satisfy a numerical target for antimicrobial use. If a country expands its meat production by 100% but only increases their AMU by 25%, it means they are using less drug per animal or per kilogram of meat. That’s a step in the right direction and a big win in my mind, as it’s often accomplished through improving overall animal health, which provides many other benefits beyond improved AMU. If a country is expanding meat production, they’re not going to sign onto any agreement that limits the overall mass of antimicrobials used, but instead we should be working together to optimize animal health in order to optimize antimicrobial use, so we maximize the benefits and minimize the risks.
Increased access to antimicriobial drugs
“Use as little as possible but use enough”. That’s my mantra when it comes to antimicrobials.
We can use too little. Animals get sick, and sometimes they need antibiotics (just like people). Internationally, a lot of animals that would be helped by an antibiotic don’t get one because the antibiotic is not available or not affordable, or there’s limited or no understanding of how/when to use it. This is most common in low income countries, but access issues in different countries vary. Improvements in drug availability, less poverty, increased literacy, improved transport infrastructue (e.g.roads), better access to veterinary care and other factors can reduce underuse of antibiotics. That can lead to a short term increase in antibiotic use, but it’s better for animal health and welfare, and hopefully is ultimately combined with improvements in animal management, preventive medicine, vaccination and other basic care.
All that said, we still need to reduce antimicrobial use
We massively overuse antibiotics (in animals and in people). However, AMR is a complex problem, and complex problems can’t be addressed with simplistic, sound-bite approaches, like picking a random number and an arbitrary date and saying “let’s reduce antibiotic use in livestock by X% by the year 20XX.” We need more nuanced discussions to maximize animal health, use antibiotics when needed, choose the right drug and duration in each case, and stop using them when they are not needed. Some of that will reduce AMU, but some might increase AMU (at the mass level or even overall), but ultimately improve overall health of animals (and people) and reduce the impacts of AMR.
We also need to think about what we really want to measure. As you can tell, I’m not a fan of measuring overall mass of drugs used. It’ better than not measuring use at all, and it can be useful in some situations, but it’s mainly used because it’s a relatively easy number to calculate. We’re better off focusing on metrics for appropriate use of antimicrobials, such as:
- The percentage of animals of a certain age or health status that are treated with an antibiotic therapeutically or prophylactically
- The percentage of treatments that are consistent with available AMU guidelines
- The percentage of treatments that use lower tier drugs
- The percentage of animals that are treated based on the advice of a veterinarian
These metrics take a lot more time to develop but are more understandable, more actionable and ultimately lead to better surveillance-to-action, and impact.